Summary
In response to an increase in women with gestational diabetes mellitus, the team developed a real-time, smartphone-based remote blood glucose management system aimed at improving the efficiency of clinical care. The system, called GDm-health, transmits blood glucose readings to a smartphone app and results are transmitted via a secure website where healthcare professionals can review the information and follow up with an SMS message to patients. 52 pregnant women used the system from June 2012 to August 2013. Satisfaction surveys indicated women were very happy with their care and the technology was reliable and fitted in well with their lifestyle.
Results
Seven women participated in the beta test phase. Changes were made to the application based on their feedback. A service development project of 52 women was subsequently conducted, 48 of them using the system until delivery. During this time 16,626 readings were transmitted.
The post-delivery satisfaction questionnaire was completed by 48 women. They reported that the technology was convenient and fitted in well with their lifestyle. The ability to monitor remotely was particularly appreciated by women with other children or who lived further away from the hospital.
Clinicians valued the improved ability to recognise BG trends, to respond quickly to women with persistently high BG readings and to recognise and contact women not performing sufficient monitoring before their outpatient visit.
Challenge
GDm (gestational diabetes) is increasingly prevalent, as pregnant women become older and heavier, with large proportions coming from high-risk ethnic backgrounds across the UK. Patient-centred care delivery must help these women understand and manage their own disease, within the context of their lifestyle.
Standard UK clincial practice is to teach women with GDm to perform fingerprick blood glucose (BG) monitoring. Management decisions rely on accurate BG monitoring.
Pregnant women with GDM are ideally suited to a digital BG management system. This age group is highly smartphone literate, and pregnant women are motivated to improve their health for the benefit their baby. The disease lasts just 10 weeks on average from diagnosis to delivery, therefor it is unlikely people will face technology fatigue.
Objectives
The aim of this service development initiative was to introduce a novel digital blood glucose management system into a maternity diabetes clinical service. Specific objectives included the development of a digital system that responds to both the needs of women with GDm and clinicians and to demonstrate the feasibility of the system as part of routine care in a diabetes in pregnancy service.
The service development also aimed to determine women’s views towards the technology, how it affected their relationship with the diabetes clinical team and their understanding of diabetes. The final objective was to analyse BG control patterns and women’s utilisation of the system.
Solution
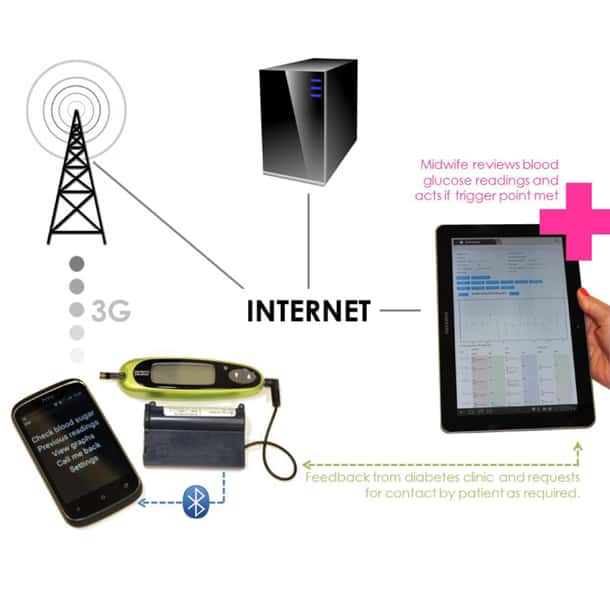
The GDm-health system was developed to transmit BG results from a standard meter via an external Bluetooth attachment to an Android OS smartphone application, enabling women to ‘tag’ readings with details in relation to meal timings. Results were transmitted to a secure website for review by the clincial care team.
A beta-test phase was conducted to confirm that the system would be reliable enough for clinical use. Technical glitches were resolved and feedback obtained. Women in this test also kept paper records.
The next phase was a service development project involving women with mild GDm. BG control was managed using the GDm-health system, without paper-based monitoring.
Measuring the effect of the GDm-health system on women’s blood glucose management was done through analysis of glucose profiles and the number of medication adjustments and comments recorded on the system. This data was extracted from the secure website after delivery.
Learnings
The key learning from this project has been the importance of strong multidisciplinary collaboration to build a system that responds to a genuine clinical need, is technically robust and is user friendly. This project is the result of a team effort, and, crucially, women with GDm have been involved at each step of the intervention development.
The concept of developing a technology ‘from scratch’ can seem daunting. In addition to drawing upon and trusting the strengths of different team members, the multiple phases of development (beta testing, pilot, and now RCT and pilot scale-up project) allowed the team to learn from a patient group at every stage and integrate improvements. This has ultimately led to the development of a culture of trust and believing in an improvement cycle as ‘usual business’.
Evaluation
The impact of GDm-health on clinical outcomes and service utilisation is currently being assessed in an RCT. The team has started to disseminate the results of this initiative through poster presentations, and have presented the project to clinicians and health service managers across our region.
Digital health solutions often face challenges in scale-up. The team is developing a model for scale-up. This will be piloted in two NHS trusts. The key challenges will be allowing for local modifications in the system whilst maintaining efficacy, providing ongoing technical support and adapting the system to enable use with other operating system platforms. Perhaps the greatest challenge will be convincing clinicians and midwives that digital health solutions can enhance clinical care delivery.