Summary
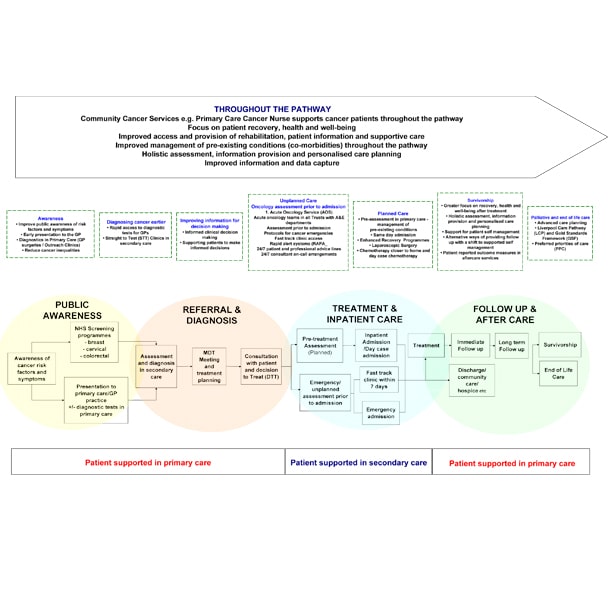
The transforming cancer care in the community (TCCC) programme was set up with the aim of establishing whether an out-of-hospital care model is scalable and sustainable; better for patients; reduces the existing over-reliance on hospital-based care; and can be more cost-effective to develop services, where clinically appropriate, outside the acute setting.
Challenge
The east of England region has 5.8 million people, just under 180,000 of them living with a cancer diagnosis. In 2012 cancer was responsible for £0.5 billion spend on healthcare in the region. This is set to rise. It is also predicted that there will be a £20-30bn NHS deficit gap by 2022. Improved services will therefore have to be provided at less cost.
Other challenges include: outcomes that are still comparatively poor nationally; a failure to deliver integrated care at-scale, outdated delivery systems, an ageing population, increasing incidence of other long-term conditions, rising ‘stakeholder’ expectation, and a wide variation in quality.
Objectives
The programme’s overarching aim was to develop a community-based model of cancer patient integrated care meeting four key objectives. Firstly, it would provide improved quality of care and achieve better coverage by, for example, offering a more responsive service and providing care closer to home.
Secondly, it should be scalable and sustainable, being designed to free-up secondary care service capacity and GP appointments, develop an integrated care pathway, and maximise the number of community-based interventions.
Thirdly, it should have a greater focus on patient and carer need, going beyond traditional treatments. Key to this was embedding the NCSI Survivorship Recovery Pack in the community setting.
Solution
A programme PID and project plan were developed, with clearly defined deliverables and success criteria. Steering groups were established for each of the seven pilots. This ensured engagement from the outset.
A TCCC evaluation sub-group was set up, reporting to a programme board which meets quarterly, and guiding the evaluation development. A partnership approach was adopted. The team engaged with the Eastern Academic Health Science Network and Macmillan.
One year into the two-year pilot phase, the East of England Strategic Clinical Network (EoESCN) evolved the TCCC Programme Board into the TCCC CCG Commissioning Forum, to establish the requirements for committing the programme to commissioning plans from April 2015.
Results
The interim qualitative evaluation report (to end June 2014) shows patience confidence in the programme at 97.5%, compared with 77.7% in the National Cancer Patient Experience Survey (NCPES). All patients reported that they ‘felt treated with respect’, compared with an NCPES figure of 82.2%. Carer confidence in the programme stood at 100%, against 68.2%.
Interim quantitative assessment found 703 patients enrolled in the service, with a total of 5221 contacts. Of those, 55 were in the GP surgery, 2,294 (44%) were telephone interventions, and 2,177 (42%) were home contacts.
Learnings
Engagement was deemed key, whether early CCG engagement or the relationship with (other) primary and secondary care teams. Visibility was also crucial to showing how the service could make a tangible difference to patient and carer outcomes.
The team found obtaining HES data for metastatic disease problematic. They also realised that remote working has limitations – teams need a central location point. There were also IT problems around remote working.
Evaluation
The service currently works with approximately 86+ GP surgeries. The programme aims to provide the evidence base to enable commissioning and to allow it to broaden the scope of patients under the care of the current pilots, spread the model across local GP practices, and ultimately across the East of England.
In parallel, adapted models are already being developed across the East of England. These include the Primary Care Practice Nurse (PCPN) programme, the Herts Valleys CCG Prostate Patient Follow-Up Programme, the Colchester Self-Managed After Care (SMAC) project, the Luton & Dunstable and St Margaret’s Hospital, Epping, Community Cancer nurse models, and the UCLH Haematology follow-up pilot.