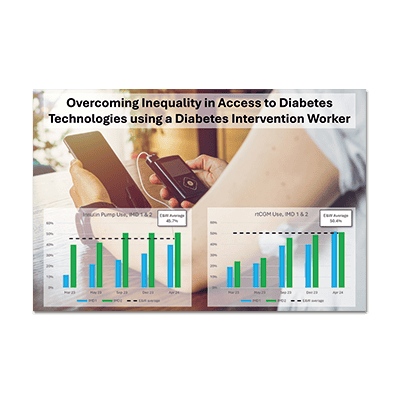
Summary
The Trust had significant inequality in access to diabetes technologies – both insulin pumps and real-time continuous glucose monitors (rtCGM) – as a result of socioeconomic deprivation scored using the Index of Multiple Deprivation (IMD) quintiles. A ‘diabetes intervention worker’ (DIW) role was piloted, seconded from the Family Intervention Service (FIS), to better understand and address barriers to technology. Interventions included direct work with young people and families, provision of mobile phones, laptops and SIM cards, plus team focus on promoting technologies to all patient groups. These actions resulted in a significant increase in pump and rtCGM use in IMD 1 and 2 (most, and second most, deprived), resolution of inequality in technology use, plus a corresponding reduction in median HbA1c.
Innovation
This one-year, NHS England-funded project employed a new staff member in a pilot DIW role, who was dual trained in diabetes technologies and family intervention work (FIS). The aims were for children and young people (CYP) with diabetes in IMD quintiles 1 and 2 to achieve the same use of diabetes technologies as E&W average levels by March 2024, to appropriately support CYP with diabetes to understand and use technologies effectively, to reduce median HbA1c for patients in IMD 1 and 2 by at least 5 mmol/mol, to build CYP and carers’ confidence in technology use, plus for the service to learn more about working effectively with families experiencing deprivation. Support was offered in patients’ homes or close to home, via telephone or video. There was a holistic approach to the work, supporting families with social needs before focusing on new technologies. Patients in IMD 1 and 2 were identified by their postcodes, and prioritised according to current use of technology and HbA1c as a clinical outcome measure. Initially the focus was on improving use of a dose calculation app, providing more real-time CGM devices (rtCGM) and insulin pump therapy. Local funding changes shifted focus to delivering more pump upgrades to hybrid closed loop (HCL) options and HCL starts. Use of rtCGM, insulin pumps and HCL systems was recorded. HbA1c was recorded at the start and end of the project. The DIW kept records to help understand common themes.
Equality, Diversity and Variation
Some families had low awareness of the technology options available. Teaching in their own homes was effective. Another issue was lack of compatible devices (eg. mobile phone/computer) and costs of data, even where a phone could be provided. The DIW secured charitable donations of 30 rtCGM-compatible mobile phones and five laptops, and 50 free data SIM cards came from a national mobile phone company. Some families thought they had to access training online, or travel (with associated costs). Here, education and training in patients’ homes helped. Where online training was essential, the DIW sat alongside patients to build confidence. Some patients needed transport to clinics or technology starts. Some young people anxious about wearable technology were helped by relationship building, home demonstrations and in-person support for the first sensor changes. The DIW worked flexible hours to support families where necessary and shared patients’ difficulties with other professionals. Most support was needed with direct, practical help using diabetes technologies. Much of the work could be delivered at lower cost by a band 4 health care assistant trained in diabetes technologies.
Results
The project saw an overall increase in use of technologies, particularly rtCGM and HCL systems, for the whole patient cohort. There was an increase from 12% to 40% of patients in IMD 1 using an insulin pump. The NPDA 2022-23 E&W average was 45.7%. IMD 2-4 also increased pump use, but the changes were smaller. There was no overall change in IMD 5. There was a reduction in inequality gap between IMD 1 and 5 from 38% at project start to 10% at project finish. There was a substantial increase in use of rtCGM in IMD 1-4 during the project, with the largest increases in IMD 1 and 2. At the end, IMD 1 (49%) and IMD 2 (51%) had similar use of these rtCGM devices compared to IMD 3-5 and to NPDA 2022-23 E&W average of 50.4%, showing closure of the inequality gap. HCL therapy was not widely available at the start of the project and, while numbers were small, there was evidence of inequality. The proportion of patients using HCL rose sharply during the project as a result of increased funding from July 2024. This improvement in access to HCL was similar over the five IMD groups. The service is currently a statistical outlier for poorer-than-expected HbA1c outcome measures compared to regional and national outcomes because of staffing difficulties and historical funding restrictions on use of diabetes technologies. One element of the action plan to address this was to improve use of diabetes technologies. Over the project year, median HbA1c reduced by 5 mmol/mol in IMD 1, by 3.5 mmol/mol in IMD 2, and by 4.5 mmol/mol for the whole cohort. The Trust extended the project for three months.
User Feedback
A survey of users has not been completed, but feedback has been positive.
Dissemination and Sustainability
The results have been presented to the two CYP diabetes teams in the Trust, the Integrated Care Board, a local Health Inequalities Board meeting, plus regional teams at the South West Children and Young People’s Diabetes Network meeting. The project showed that there were significant benefits to be gained from a dedicated practitioner offering holistic care, and that there is a case for embedding key areas of learning into local practice. The intention is to review the feasibility of future team roles with flexible hours and increase face-to- face outreach options in service delivery. IMD quintiles will be included in quarterly reviews of data on HbA1c and technology uptake and noted for each patient when planning support. There is an ongoing need for sustainable sources of allied technologies. It would be relatively straightforward for another service to implement a similar initiative, using a healthcare worker with similar remit, or an allied worker with a social care background.