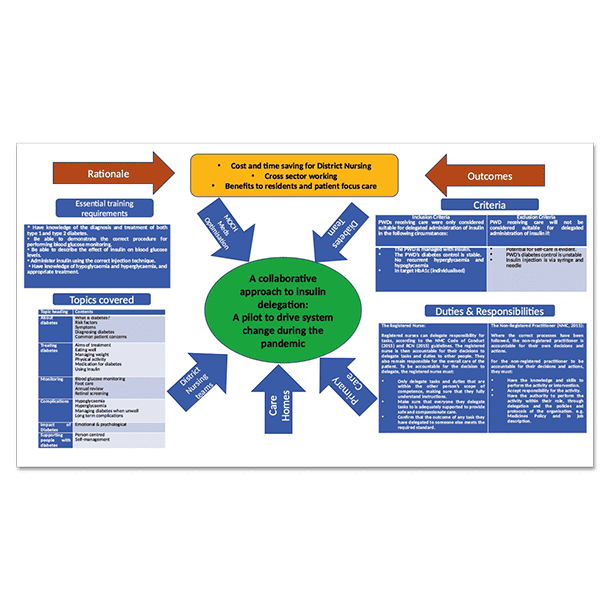
Summary
The rising number of older, frail, and co-morbid people with diabetes requiring insulin therapy via community services put additional pressure on overstretched community nursing workloads, especially during the COVID-19 pandemic. Therefore, appropriately trained and competency assessed health support workers and healthcare assistants were identified to administer insulin to people with stable diabetes control. Joint working, led by East Sussex Healthcare NHS Trust with Sussex Community NHS foundation Trust, prior to the launch of the NHSE and NHSI framework, resulted in a draft guideline to enable these workers in residential/care homes to administer insulin using pens to adults with diabetes.
Innovation
The pandemic unearthed areas of concern regarding the management of PWD in the community, especially for those requiring regular support from community nursing teams. Numerous factors impacted the administration of insulin and capillary blood glucose monitoring, including delays and unintentional omissions due to increased workload pressures, IT problems, lack of staffing/resources, and traffic. This pilot demonstrated that safe delegation of insulin administration to health and care workers released the capacity of community nurses, reduced unnecessary delays in delivering insulin to people with diabetes (PWD), improved cross-sector working, Medicines Optimisation in Care Homes (MOCH), empowered the care home role, improved the quality of patient care and supported resilience of the community workforce. This was demonstrated through quantitative data and qualitative feedback from staff and service users. Fourteen care homes and one for respite care in East Sussex were included in the pilot. They had PWD under the caseload of the community nursing team, who visited at least daily, and up to four times daily, depending on the insulin regimen, for administration of insulin and blood glucose monitoring. A total of 22 PWD satisfied the criteria, requiring a total of 46 daily visits by the community nursing team to administer insulin. Online training was completed by 90 staff from the care homes prior to face-to-face assessment of competency. They were also given a resource pack for reference. Competency would be checked at least once per resident and, typically, three times for a new carer/resident every two years. Assessment in practice must be by a Registered Nurse with competence at level 4 or above.
Results
The pilot achieved the following benefits: 1. Cost and time saving for community nursing. The community nursing team spent an average 30 minutes per visit on monitoring capillary blood glucose and insulin administration. The 22 PWD in the pilot received this care from the HCWs in their respective homes. For 46 visits a day, of 30 minutes each, this equates to 8,395 hours a year. Using another 30 minutes to assess the competencies of the HCW three times per PWD before being signed off equates to 2,970 hours a year. This results in 5,425 hours a year of visits saved from the community nursing caseload that could be diverted to look after more vulnerable people in the community. The Agenda for Change Band 5 mid-point is £27,239 pa. The gross hourly income before tax is £13.93. Calculating the cost of the visits (5,425 hours) a year using the hourly rate of a mid-point Band 5 RGN equals £75,570. Incorporating the time spent in providing training and assessment of the HCWs still results in significant cost-positive implication. Furthermore, this does not include the mileage costs. 2. Cross-sector working. The pilot was designed in close collaboration with the community nursing teams, health and social representative, diabetes specialist team and MOCH. This ensured multi-sectoral discussion and agreement on improvements. 3. Benefit to residents and patient-focused care. Numerous incident reports had identified delays in the delivery of insulin, with contributing factors including task allocation, heavy caseloads and traffic. Trained and assessed HCWs provided this care without such delays. The HCWs also had closer professional relationships with PWD. Their presence in the care environment where the intervention took place also reduced, if not avoided, issues relating to the incidence of acute diabetes complications.
User Feedback
Community nurses, care home managers, residents and next of kin all reported positive experiences from the pilot.
Dissemination and Sustainability
The pilot significantly reduced the number of visits from the District Nursing caseload. It enhanced cross-sector working, reduced delays in the timing of insulin administration and improved access for patients, especially against the background of the COVID-19 pandemic. It will continue after the pandemic period. A full guideline has been developed for local use and adheres to NHSE best practices. The success of the local pilot brought support from key stakeholders and reassurance in terms of risk management. This enabled the team to take up the NHSE voluntary framework and obtain governance and accountability sign-off through the local Trust. Close working with key stakeholders from the outset helped overcome challenges that others had struggled with, mainly around governance processes. This prevented several neighbouring areas from starting this work. It was vital to engage the Head of Community Nursing employed by East Sussex Healthcare, the organisation which supplies community nurses. This work is being considered at Sussex level. The framework is easily transferrable to other service