Summary
The key to reducing diabetes-related amputations is to ensure that an integrated footcare pathway is in place and there is access to a multidisciplinary foot team. Sheffield, in 2009, had all of this – yet it still had one of the highest amputation rates in the country. Root cause analysis of all amputations over a 12-month period identified that the sheer complexity of the pathway was often creating unnecessary barriers to the patient journey. A number of different initiatives, were implemented, such as a foot hotline, simplification of the foot pathway and improved training of primary care screeners. As a result, there has been almost a halving of the amputation rates in Sheffield, over a period when the national rate has remained static.
Results
The overall amputation rate in people with diabetes has fallen from 4.4 to 2.7 amputations per 1000 people with diabetes (2007-10 vs. 2010-13). Major amputations over this period also fell from 1.75 to 0.9 amputations per 1000. Other surrogate markers of the quality of care, such as the number of days in hospital for diabetic foot problems fell from 265.4 to 170.9 days. There have also been many qualitative benefits: the foot hotline receives between 10-20 calls weekly and has been universally popular with healthcare professionals in the community. Every contact through the hotline is an opportunity for education, and intervention or treatment can commence even before the patient has been seen by the MDT team. The restructuring of the diabetes foot clinics has led to the ability to review patients with a foot care emergency throughout the whole week.
Challenge
Amputation is one of the most feared complications of diabetes and has an enormous impact on patients’ lives, including loss of occupation and status, disfigurement, reduced mobility, and depression. In addition survival is bleak, with mortality rates after amputation of 50% at five years, which is worse than many cancers. A recent study has shown that there is a 10-fold variation in the incidence of major amputation as a consequence of diabetic foot disease. Sheffield had one of the highest amputation rates in the country from 2007-10: 4.4 amputations per 1000 people with diabetes, compared to a national average of 2.7. In addition, from 2008-12, there was an 80% rise in foot clinic activity (reflecting the increasing prevalence of diabetes from 4.2% of the population to 6%), without the equivalent rise in resource - and this was resulting in significant levels of both patient and staff dissatisfaction.
Objectives
After a detailed root cause analysis of every amputation (minor and major) over a 12-month period, it became clear that there were issues across both primary and secondary care which were potentially contributing to our high amputation rates, with at least 20% of them potentially avoidable. No single intervention was likely to be effective so the team set out to design and implement a series of different interventions that would result in the primary objective of reducing the rate of amputations and secondary objectives of reducing delays and improving patient experience.
Solution
A steering committee was set up with representatives from primary care (medical and nursing), the PCT/CCG, podiatry, vascular surgery, diabetes nursing, administrative staff and patient representatives. Many meetings had external facilitators, with expertise in skills such as service mapping. Some of the key interventions were:
- Introduction of a diabetes foot hotline, carried by a consultant diabetologist, to provide immediate advice to any community healthcare professional and enable fast-track to the MDT foot clinic.
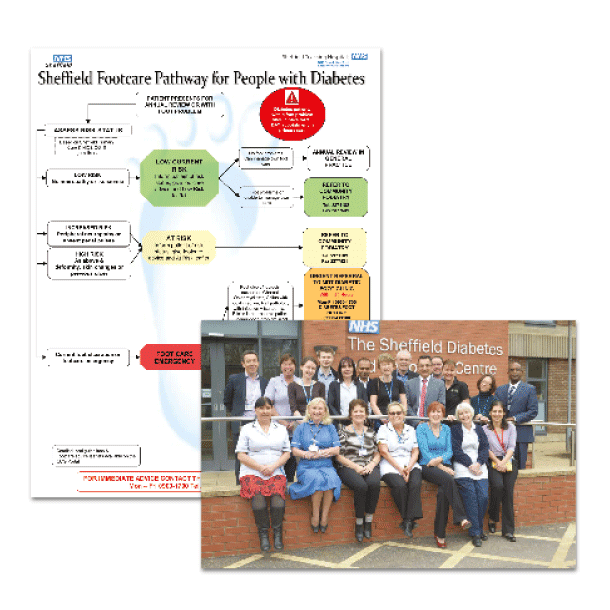
- Simplification of the footcare pathway and a single point of referral for all foot-related referrals
- Improved access to training for primary care screeners, including the development of a community-based diabetes podiatrist whose role was to target GP practices with training needs
- Improved education of patients, including the development of specific leaflets which included important contact telephone numbers
- Closer liaison with microbiology, including detailed protocols for surgical and wound swab specimens and consultant microbiologist presence in MDT meetings
Learnings
It is not enough to have the appropriate structures in place. Foot care pathways are complex healthcare systems that cross organisational structures and these structures often create unnecessary barriers within the patient journey. By analysing the entire pathway and focusing on the patient journey, the team has come up with innovative strategies that are more effective than focusing on individual departments or functions. Many of the key problems and issues we identified are likely to resonate in many other areas of the UK. Identifying these issues and developing appropriate solutions is not always straightforward. The challenges of meeting or overcoming the competing needs of different services, commissioners and providers should not be underestimated. The team feels the strategies and tools that they have used to overcome these challenges could be adapted by others within their services. It would enable them to better understand what parts of their pathway add value to patient care, simplify processes and ultimately reduce the incidence of this devastating complication.
Evaluation
Patient feedback has also been significantly positive, with a recent survey showing over 90% satisfaction with the service provided. Staff morale has also improved dramatically.